The 24th edition of the International AIDS Conference (AIDS 2022) closed this past Tuesday in Montreal (Canada) with optimistic messages about the global fight against this endemic disease, but also with clear signs of concern as a result of the latest published data, which they indicate setbacks in the progress achieved in previous decades.
One of lime and one of sand, a celebration and a complaint. This is how the week has passed in which it is considered the largest global event for the community that works to end HIV, an event that is held every two years under the auspices of the International AIDS Society (IASociety).
The Government of Canada, the host country, has denied visas to many of the participants and delegates, especially those from countries in the global South. Even before its inauguration, the outgoing president of the conference, Adeeba Kamarulzaman, loudly expressed during a press conference the concern that has been on the minds of many in recent times: the risk that the world will deviate from the path in the fight against HIV and not because there is no information or resources, but because what should be done is not done.
“We are seeing over and over again that, whether in the context of HIV or COVID-19, too many public health decisions are based on politics and profit, rather than scientific advancement and input. of the most affected”, he criticized.
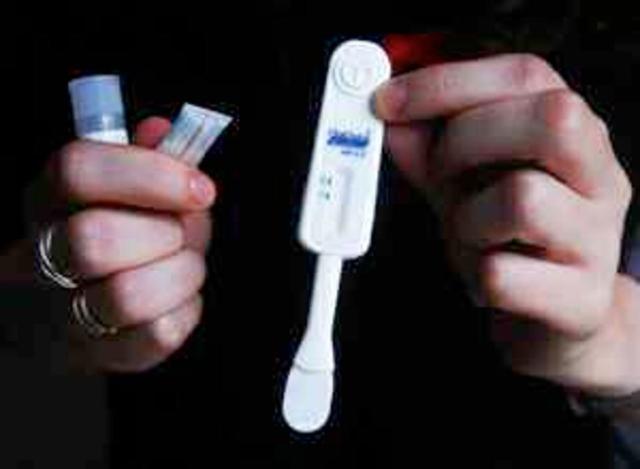
Alarming statistics
Not only because of the new coronavirus pandemic, but also because of the impact of the Russian invasion of Ukraine, the truth is that the most recent data presented by the United Nations is not very encouraging: 1.5 million new infections and 650,000 deaths in the which has been the year with the slowest progress since 2016. In addition, increases in cases have been found in almost all regions of the world.
The conference wanted to be a platform in which the international community renews the vows of its commitment to the global response against the virus, as made clear by the slogan chosen for the event: “Re-engage and Follow the Science”: commit yourself and follow science”.
During these five days, brushes have been given on the future research agenda, new prevention tools, improved treatments and possible steps towards the end of this still incurable immunological disease have been shown.
“In these highly polarized and politicized times, this message is incredibly important. Our goal this week was to focus minds on people’s needs and new scientific evidence. Politics and policies must be designed around these two pillars and in that order”, Jean-Pierre Routy, co-chair of the conference, claimed during the closing ceremony.
The Visa controversy
Not only AIDS has been discussed at a meeting that should have served that purpose, since the Government of Canada, the host country, has denied visas to many of the participants and delegates, especially those from countries of the global South, such as the activist Tia Johnson, founder of the African Alliance for HIV Prevention.

“I am deeply upset by the high number of denials and visa backlogs that have prevented many registered delegates, including IASociety staff and leadership, from entering Canada,” Kamarulzaman complained at the opening ceremony, attributing the difficulties of those attending a problem of “global inequality” and “systemic racism“.
Winnie Byanyima herself, director of the United Nations Program to Fight HIV (UNAIDS) denounced the barriers she also encountered with a tweet: “I am at the Geneva airport, at the boarding gate, with the boarding pass in hand on the way to #unaids2022. I was almost denied boarding, with all the documents reviewed over and over again, the calls made… I boarded the last one. Hundreds of people in the South have been denied visas and will not attend. Unfair, racist!” she wrote.
A step forward in prevention
The priority is to ensure that new advances quickly reach those who need them most, primarily in low- and middle-income countries, as well as key populations such as sex workers and injecting drug users. For this reason, one of the findings that has received the most attention has been the new way of preventing HIV infection through the use of pre-exposure prophylaxis (PrEP).
Oral PrEP was first approved in the US a decade ago, but acceptance and adherence have been limited, in part, by the fact that some people have difficulty taking daily pills. In recent years, a pair of studies known as HPT083 and HPT084 have shown long-acting Cabotegravir, or CAB-LA, given by injection once every two months, is a safe and effective alternative to oral PrEP.
Within the framework of this congress, the conclusions of both have been presented, which analyze the effectiveness of CAB-LA, in cisgender men and in transsexual women the first, and in women, the second. In all cases, the injectable version was more effective than the oral one and, in the case of trans women, it is also observed that the medication does not interfere with gender-affirming hormone therapy.
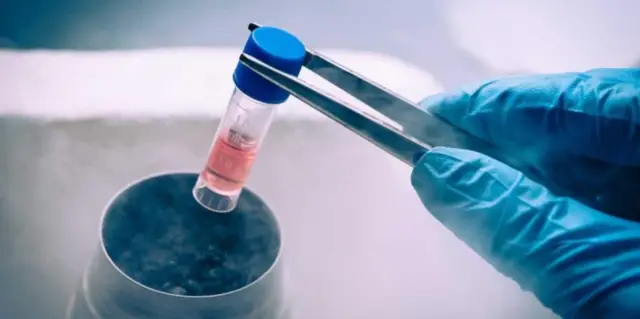
With the intention of making CAB-La widely available, two new strategies were also announced at this conference. The first, an agreement between ViiV, the pharmaceutical company that manufactures it, and the UN Medicines Patent Fund so that generics can be manufactured and access to the drug is affordable in 90 low- and middle-income countries in the world with the highest burden of the illness.
There are still big questions to answer about this agreement, since questions have been left up in the air, such as what will happen to a large number of middle-income countries that have not been included, especially in Latin America, where there are millions of people who could benefit from the medicine.
The second announcement, this one from the WHO, has been a CAB-LA recommendation as an additional HIV prevention option for people at considerable risk of contracting it, who are 70% of those newly infected each year: construction workers, men who have sex with men, injection drug users, prisoners, transgender people and their sexual partners.
New pathways to a possible cure for AIDS
In the field of advances aimed at curing AIDS, the cases of those known as the Barcelona patient and the London patient have also been presented. The first is a woman from the Catalan capital who has managed to live for more than 15 years without a viral load and without taking antiretroviral therapy. The team that has handled her case, led by doctors from the Hospital Clínic of Barcelona, have also found out what cellular mechanisms have made functional healing possible for women.
Just as optimistic is the story of the so-called City of Hope patient, a 66-year-old man who was diagnosed with HIV in 1988. In 2019, he developed acute myeloid leukemia and received a stem cell transplant from a donor who was naturally resistant to HIV. Thirty-nine months later, the man has no detectable HIV DNA in his body, so he appears to be cured.
This is the fourth known case of remission in an individual who received a transplant, and its peculiarity is that the donor and the recipient were not perfectly compatible, which indicates that this option could be available to more patients. “Although transplantation is not an option for most people with HIV, these cases remain interesting and inspiring, and help illuminate the search for a cure,” said Sharon Lewin, newly elected president of the IASociety and Kamarulzaman’s successor. The fourth known case of complete remission of HIV in a bone marrow transplant patient was presented at the conference
Another of the advances presented is a more effective way of treating HIV and hepatitis B patients, who account for 7% of the world’s population. The success of a new strategy to prevent sexually transmitted infections or STDs through the so-called Doxy PEP, which is short for doxycycline post-exposure prophylaxis, was also presented. Doxycycline is a safe and widely used antibiotic, and research found that taking it within 72 hours of having sex without a condom reduces the risk of three Bacterial STDs: gonorrhea, chlamydia and syphilis. However, more research is still needed to better understand the potential impacts on antibiotic resistance.

Among the most positive news, the success of Botswana, which has managed to comply with UNAIDS’ 95-95-95 strategy, that is: that 95% of the population suffering from HIV is diagnosed; that 95% of them are on antiretroviral treatment, and that 95% of these do not have a detectable viral load. Botswana has a very high prevalence – one in five adults is HIV positive – but the country has put in place a number of strategies such as Test and Treat which provides immediate antiretroviral therapy to those who test HIV positive.
An alliance against childhood HIV
The Montreal meeting has provided a platform to announce new agreements, such as the new Global Alliance to End HIV/AIDS in Children by 2030, led by UNAIDS, UNICEF and the WHO, and the governments of some of the most endemic countries.
It is propitiated by the fact that only 52% of children living with HIV/AIDS are receiving treatment –among adults, the world average is 76%– and its goal is that, by the end of the decade, no minor with HIV/AIDS are denied treatment and that all are born without the virus. Among the most urgent points of action is care in prevention, diagnosis and treatment of pregnant and lactating women and adolescents, as well as guaranteeing comprehensive care for babies, children and adolescents who carry HIV or who are exposed to it.

For those who have experienced shifts in consciousness and know that more peace, joy, and love awaits in a better living environment. A bold shared vision. A living community and hub for innovation. A sustainable ecosystem for living and working. A model for the new future.
